Periodontitis versus Peri-Implantitis - Pathogenesis and Treatment Options - Congress Lectures - Home
Periodontitis versus Peri-Implantitis - Pathogenesis and Treatment Options
The aim of this lecture is to discuss similarities and differences between periodontal and peri-implant tissues, which affect the pathology, disease diagnosis and consequent treatment modalities.
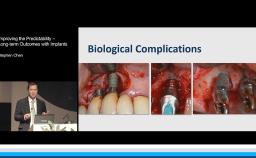
Clinically, peri-implantitis is associated with deepened pockets, bleeding on probing and/or suppuration and the loss of supporting marginal bone. Similar to periodontitis, the major etiologic factor is the microbial biofilm, and both implant components and implant restorations should be designed so that personal oral hygiene is feasible.
Patients should be informed that peri-implant tissues respond to plaque accumulation in a similar way to periodontal tissues, and that disease may develop in the tissues around the implants, which would jeopardize their longevity.
Adequate personal oral hygiene is essential and patients with a history of periodontal disease, in particular smokers and those suffering from diabetes mellitus, should be informed about the increased risk of peri-implant disease before implant placement. It is imperative that periodontal disease is treated before implant placement.

- Duration
- 57 minutes
- Source
- ITI Congress Australasia 2013
- CPD/CME
- 0.95 hours
- Purchase price
- 29 Academy Coins
Share this page
Download the QR code with a link to this page and use it in your presentations or share it on social media.
Download QR code